|
Difference between vasomotor and other symptoms of menopause
By Monazza Ahmad, B.Pharm, MSc Menopause is undeniably the most confusing phase of a woman’s life. The irregular menstrual cycle and unpredictable biological changes and emotional state can negatively affect her social, work, and daily life. Seeking help for these symptoms could feel awkward since many times women don’t know how to communicate these concerns and whether it would be empathetically understood or not. At times, the complex medical terms associated with menopause can make it tough to follow the course of treatment plan. Let’s discuss the major signs and symptoms of menopause and the terminologies associated with it that may help you understand your situation as well as convey your concerns to your provider. What are vasomotor symptoms (VMS)? The word “vaso” is originated from the Latin1 meaning vessel, and “motor” relates to movement. So vasomotor symptoms are the movement of blood vessels characterized by their constriction and dilation that causes temporary irregular blood pressure that in turn alters the body temperature, making us feel hot or sweat.2 This temperature alteration results in hot flashes and night sweats that are the most common indication of perimenopause and menopause.3,4 Other chronic and progressive symptoms are characterized by vaginal dryness, painful intercourse, and reduced lubrication. It is seen in both premenopausal and postmenopausal phases.5 Why do I feel like I’m the only one suffering from these symptoms? During menopausal transition, the vasomotor symptoms impact about 80% of the women in the US and differ widely from region to region.6,7 Even though a variety of symptoms is common during menopause, some are not much reported due to their mild and nonspecific nature. Up to 84% of postmenopausal women tend to just deal with the menopausal discomfort rather than seeking medical attention.5,8 How long do these symptoms last? Don’t worry if you have been experiencing vasomotor symptoms for more than a few years. For many women, it can last over a decade or two, with 4-20 hot flashes daily being common during menopause.9 A new long-term study of women from various races and ethnicities suggests that hot flashes and night sweats can take up to 11 years to resolve for some women. Interestingly, the study further discovered that hot flashes lasted longer, for 9-10 years, if started before the menstrual period ended, while their duration was much shorter, with 3.5 years if women had their first hot flash after the periods ended.10 Some menopausal symptoms can get worse with age as opposed to the other menopausal symptoms that improve with time. How do these symptoms impact women’s quality of life? Hot flashes, night sweats, vaginal dryness, low libido, sleeplessness, and menopausal anxiety all add to the decline in quality of life. The sudden outburst of sweat with hot flashes can be daunting when it occurs in a gathering, making women nervous. Vaginal dryness and decreased interest in sexual activities go hand in hand, impacting intimate relationships. All of these stressful changes in daily routine are enough to make any woman anxious.5 Some of the other concerns include brain fog, urinary incontinence, weight gain, hair loss, bone loss, and heart health, to name a few.11 Therefore, women are highly encouraged to not ignore menopausal discomfort and instead have informed discussions with their healthcare providers to find safe solutions for their health needs.12 What are my relief options? There are several options to reduce the impact of these menopausal symptoms and claim your lifestyle back. The solutions include prescription medications, well-studied supplements, lifestyle changes, and nutrition. Since the trial and error of wrong choices can become painful and lengthy during menopause, it is important to discuss the best option with your provider at the right time. Hormone replacement therapy (HRT): This is the most common prescription option for hot flashes, but it is not usually the first choice. The common forms are tablets, gels, skin patches, injections, and vaginal inserts. HRT is generally best-suited for healthy women and those that are in the early phase of menopause. It is not recommended to start HRT after the age of 60. However, there are some side effects associated with HRT, and it is generally considered unsafe for people with a history of heart conditions, deep vein thrombosis, cancer, and smoking.12 Rheum rhaponticum (ERr 731®): This nonhormonal solution is the top recommended natural ingredient by OBGYNs. It has shown to improve 12 of the main menopausal symptoms by 83%. In addition to hot flashes and night sweats, it also improves sleep disturbances, mood swings, sexual discomfort, anxiety, vaginal dryness, and muscle and joint health, to name a few.13 Lifestyle: Daily physical activity is important for menopausal symptom relief. Weight management, stress relief, increased metabolism, and improved overall quality of life as a result of active movement are all related to better management of menopause.14 Eating habits, consuming a healthy diet, practicing relaxation or meditation, drinking enough water, getting quality sleep, and avoiding smoking and alcohol all help with relieving the menopausal discomfort.15 Nutrition: Taking necessary supplements or eating food rich in vitamin D, E, B6, folic acid, and omegas help reduce intensity of menopausal symptoms.16 Now that you have learned more about menopausal symptoms and their treatment options, you may want to discuss these concerns with your healthcare provider. In our next post, we will go over a few tips on how a patient and their healthcare provider can effectively communicate these menopausal challenges with each other to come up with the best treatment plan. References:
0 Comments
By Monazza Ahmad, B.Pharm, MSc To ensure best health outcomes in a healthcare setting, it is important to establish open, effective, and respectful communication between a patient and a healthcare practitioner. As a patient, it is not only your right but in your best interest to ask your doctor for clarification or further explanation on your health condition and treatment plan. As a healthcare provider, it is your responsibility to provide a safe and comfortable environment for your patients to openly discuss their health concerns and make sure your diagnosis and treatment plan is well understood. That said, menopause can trigger many complex and confusing symptoms that can be uncomfortable to talk about, which can make managing the symptoms difficult. Here are some tips for both patients and practitioners to start the conversation around menopause and its symptoms that we discussed in our previous post, Menopausal Symptoms. When should I talk to my doctor about menopause?1 First of all, don’t feel awkward. Menopause is a natural phase of life, and your doctor is likely familiar with all possible symptoms. Describe your condition and symptoms in detail and explain how they are affecting your lifestyle and relationships. The provider needs to rule out any other underlying conditions before determining it is menopause. Reach out to your doctor if:
Don’t forget to tell your doctor if you have any allergies or other health conditions. Also mention any medications or supplements you’re already taking for menopause symptoms or other conditions. What shall I ask my doctor? Medical appointments can be stressful, and we often feel rushed. When you have a delicate issue to bring up, being prepared can help. Here are some of the questions you can ask your practitioner:
How can healthcare providers ensure the right care during menopause? Often, the reluctance from healthcare professionals to address these female issues can also cause lack of awareness. It is the healthcare provider’s obligation to make sure patients feel comfortable in discussing their menopausal concerns and understand the treatment plan.2 According to a survey by NIH, patients are likely to discuss menopause transition with providers who don’t make them feel rushed, are good listeners, and have expertise in this area of women’s health. Here are some ways to help your patients receive the best care:
What to ask your patients:3
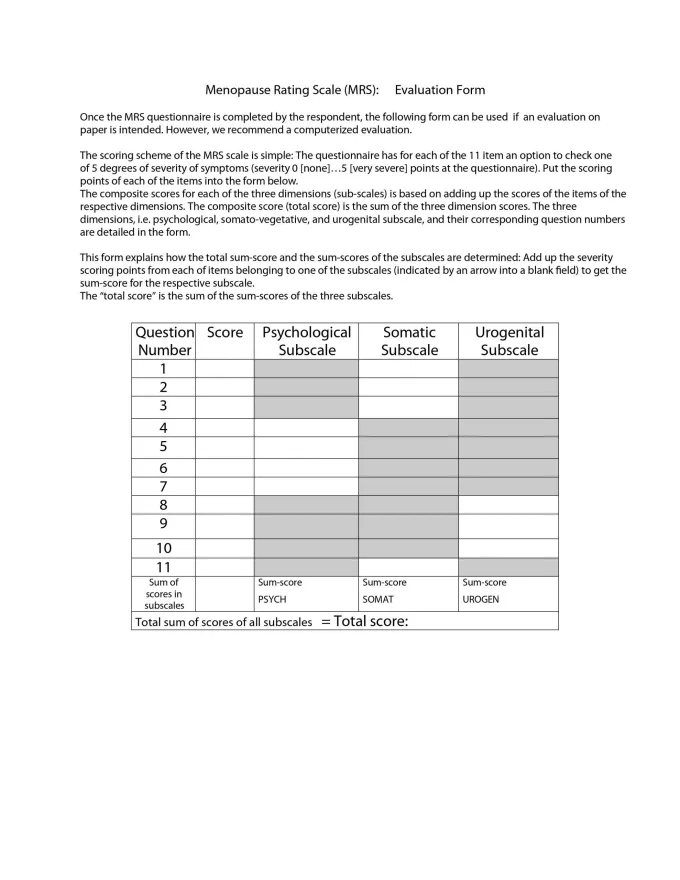
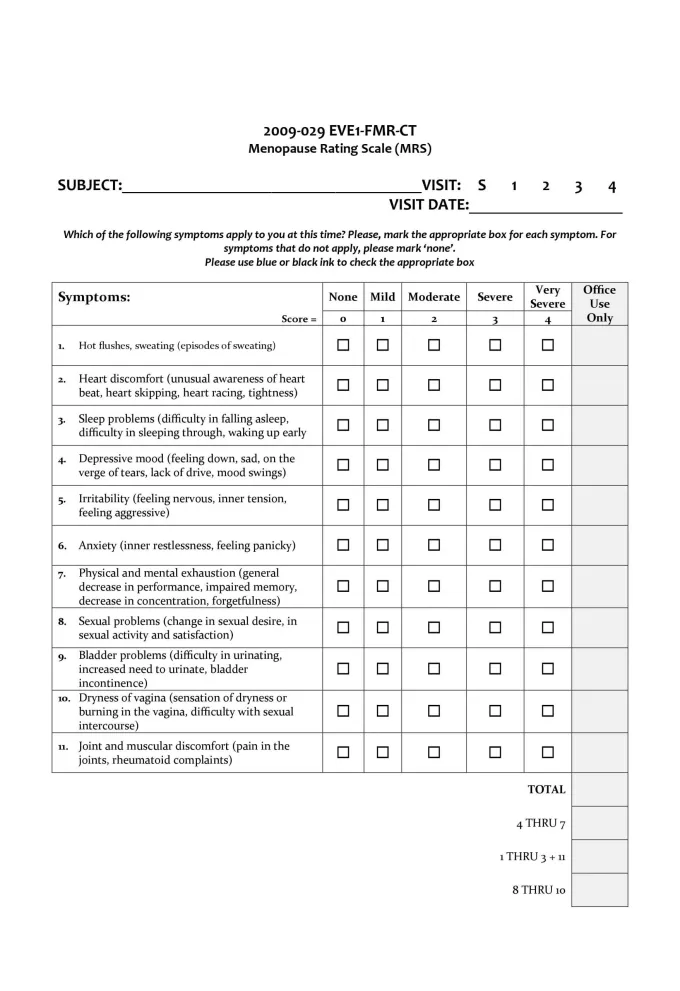
Menopause symptoms evaluation form and rating scale (click to enlarge)Menopause is a natural phase in a woman’s life, and its challenges need to be accepted and understood at work, at home, and on a social as well as a societal level. Unless these concerns are progressively communicated in a healthcare setting, it will be tough for us to understand the impact of this condition on a woman’s life.
References:
|
Categories
All
Archives
April 2024
|
|
Join Our Community
|
|
Amipro Disclaimer:
Certain persons, considered experts, may disagree with one or more of the foregoing statements, but the same are deemed, nevertheless, to be based on sound and reliable authority. No such statements shall be construed as a claim or representation as to Metagenics products, that they are offered for the diagnosis, cure, mitigation, treatment or prevention of any disease. |





 RSS Feed
RSS Feed