|
It’s not all fun and games when you’re living the low-carb lifestyle—but sometimes, it can be! Read on for a list of low-carb cocktails you can enjoy while following a ketogenic diet plan. First, here’s a simple rule of thumb: when consumed in moderation, any hard liquor can be considered acceptable by keto standards—either by itself or with plain, sugar-free sparkling water. Many sparkling waters contain zero everything, including calories, sugar, sodium, and, of course, carbs; just make sure you check the label or ask the bartender. For extra flavor, fresh lemon or lime juice is always acceptable. Whether you’re at home or at happy hour, these seven “ketolicious” cocktails won’t disappoint. Vodka Soda: A simple, low-carb favorite.
What you’ll need:
Some like it sweet You don’t have to sacrifice sweetness in your low-carb cocktail fix. Each serving of this ketogenic simple syrup contains just 2 net carbs. What you’ll need:
Remember: If you choose to indulge in alcohol, it should always be in moderation. Enjoy responsibly. With all the keto-friendly cocktail options out there, you have yet another reason never to feel like you’re missing out on anything. Cheers!
0 Comments
The ketogenic diet has helped countless people who have struggled with managing their weight. But it is a diet that has now been split into two different diets: one diet’s been around for over 100 years; the other is a new spin for modern eating habits: How do you decide whether eating clean versus dirty keto is the right diet for you? Compared to the Standard American Diet (SAD), clean keto is not only used to help people lose weight, recent studies have also demonstrated it hosts a variety of health benefits that don’t include weight loss: Clean keto can help increase energy levels, promote brain function, and support athletic performance—for both professionals and amateurs alike.1 Those who have experienced the benefits of clean keto are understandably curious about the latest version of the diet, known as “dirty keto,” and how it holds up against eating clean. Let’s take a closer look.
Keeping it clean. The clean keto diet is based on the idea that eating a fixed macronutrient breakdown of mostly healthy fats, high-quality protein in moderation, and restricted carbohydrates (less than 50 grams per day) provides your body with the fuel you need to lose body fat without hunger, weakness, and fatigue.2 The reduction in carb intake puts your body into a metabolic state called “nutritional ketosis.”3 During this nutritional ketosis, your body no longer relies on glucose as a primary energy source. Instead, your liver converts fat into ketones–which are a great source of fuel for both your body and brain. Ketones also increase the brain-derived neurotrophic factor (BDNF), which works to support your brain’s existing neurons while encouraging new neuron and synapse growth.4 On the clean keto diet, you get most of your calories from healthy fats found in foods like avocados, grass-fed butter, olives, olive oil, coconut oil, nuts, and seeds. However, keep in mind that some nuts and seeds are better than others. You’ll want to choose those that are high in fats and lower in carbs; brazil nuts, almonds, walnuts, chia seeds and flaxseed are all good options. You can also eat all of the nonstarchy, leafy vegetables you want, as well as other low-carb vegetables like broccoli, peppers, cauliflower, green beans, asparagus, cucumber, and zucchini. In moderation, eat protein in the form of grass-fed meats, pasture-raised poultry, cage-free eggs, and wild-caught fish. Finally, if you want to reach for something sweet, 90% dark chocolate is your best option. On the list of what not to eat? For starters, remember that the clean keto diet restricts the intake of carbohydrates to achieve a shift from glucose to ketones as a primary fuel source. In order to avoid food high in carbs, limit fruit consumption—as it’s higher in sugar content–and forego fruit juice altogether. You should also avoid grains or starches such as rice or pasta, beans or legumes, root vegetables, and any low-fat or diet products, as they are typically highly processed and high in carbs. Let’s talk dirty (keto)Dirty keto follows the same macronutrient breakdown of fats, protein, and carbs as clean keto, with one major difference: It doesn’t matter which foods those macros come from. That is to say, on the dirty keto diet, instead of choosing good fats, like wild-caught salmon, grass-fed butter, and avocado, you eat a fast-food burger (without the bun), processed cheese, and pork rinds. Can you lose weight by following the dirty keto diet? Possibly. But the benefits halt there—and there are remarkable health drawbacks from the dirty keto diet that you should be aware of, too. For starters, this keto diet is missing vital micronutrients like vitamins, minerals, and enzymes that are necessary to your overall health. Furthermore, processed foods are usually high in sodium, which can lead to bloating and inflammation. You’re also more likely to regain the weight you lost and experience more cravings and less satiety. Dirty keto foods can trigger these cravings, bloating, and feelings of withdrawal which are symptoms commonly associated with what is known as the “keto flu.” You are what you feed your brainIn a healthy digestive system, the cells that form the paper-thin lining of the small and large intestines are packed very closely together. In fact, they’re so close that under normal, healthy conditions, only digested food (solutes) and water—can and should—enter the bloodstream. But when there is intestinal inflammation or inappropriate dietary intake, the tight junctions of the gut lining can easily be disrupted and become too porous. Diets high in chemical-laden processed foods—such as those often consumed on the dirty keto diet—can damage the gut lining and force it to become more permeable. These same factors also affect the balance of both the trillions of beneficial and harmful bacteria in the gut. When this balance is disturbed, harmful bacteria can get the upper hand and cause an increase in gut permeability. The result is intestinal hyperpermeability, or “leaky gut.” This condition can allow toxins, bacteria, undigested food particles, and other undesirable gut contents to enter the bloodstream and circulate to the rest of the body, including your brain. Not only does your gut affect your mental state in how you feel physically, but the reverse is also true: Your mental state affects your gut and gut health. This makes following the clean keto diet a better choice for your brain’s health. While dirty keto follows the same macronutrient breakdown as clean keto, there are marked differences in the two diets and their respective impacts on the body (and brain). A dirty keto meal can be a placeholder while you’re in a pinch, but it shouldn’t be part of an ongoing healthy eating regimen. Instead, by following a clean keto diet, you’ll not only find success losing weight and gaining energy, but you’ll also provide your brain with longer-lasting, healthier fuel. References:
How many of your patients complain of fatigue and lack of energy? These symptoms may be indicators that your patients might benefit from a metabolic detoxification program. Metabolic detoxification is the body’s natural ability to metabolize, neutralize, and excrete potentially harmful substances while temporarily reducing incoming potentially harmful chemicals or pollutants. A metabolic detox program supports this natural process when the body is unable to keep up with its toxic load.
Why detox? It’s not just a fad. Metabolic detoxification supports liver function and can help patients shift poor dietary habits, and since they may feel an immediate difference, it can help improve compliance. Setting up a group detox connects patients with similar needs and desired outcomes, and it may benefit the practitioner as well: Since group sessions allow for cost sharing, it’s more affordable for the patients, which can inspire more patients to participate. Get started. You can determine which patients will benefit most from a detox by having them respond to a detox screening questionnaire. This could be used as a subjective review of the patient’s systems along with your physical examination to determine to what extent detoxification support may help and the ideal duration of detoxification. You’ll also be able to use the responses as a baseline to evaluate progress following the detox protocol. Based on the number of patients who express interest in learning more, set a date and location for your presentation. Create a flier to hand to patients or leave at your front desk. Print out a sign-up sheet for patients to register immediately before or after a clinic visit. Promote the session on your social media and sharing sites. Suggest that your patients invite their spouses or friends if they feel they would be interested or may be good candidates. As an incentive, you might consider waiving the registration fee for patient partners. Finally, order enough detox kits to have on hand for purchase based on the number of attendees who register. Remember, people will be more likely to participate in the group detox if they can start quickly and don’t have time for their excitement to wane. Create your presentation. As you pull your presentation together, there are several elements that should be included:
After the event. Create a group email list or a social media site where patients can regularly “check in” with you (and one another) for added support during the detox process. This added social support and encouragement is helpful for successful outcomes. Follow up with patients several times during the process as well as afterward to get feedback on their progress and to get feedback for future group detox events. Additional event tips. In addition to guidance provided throughout this post, here are a few additional tips to help you and your patients get the most out of the event:
Ready to get your group detox started? Follow these guidelines to help ensure it’s a success! Submitted by the Metagenics Marketing Team Many of us (men and women) have had moments where we sneezed and lost control of our bladder, or we had a coughing attack and sprang a little “leak.” But for women in menopause, urinary leakage can occur more frequently and cause embarrassment and concern. Urinary incontinence is actually common during this time in a woman’s lifespan and can be the result of one or more causes. Fortunately, there are many ways to address this problem.
What is urinary incontinence?Simply put, urinary incontinence is the involuntary leakage of urine.1 Up to one-third of men and women in the US have urinary incontinence,1 but it is older women—those going through perimenopause and menopause—who most often develop stress urinary incontinence (SUI).1 Urge incontinence (UI) is also common in postmenopausal women; also known as overactive bladder (OAB), the condition results in a fast, urgent need to urinate, accompanied by urine leakage.2 Bend. Lift. Leak.As time marches on, children are born, and estrogen levels drop, the pelvic floor muscles that support the bladder and other organs can naturally weaken and become stretched. Less support means less ability to hold urine, and when the urethra (the duct where urine comes out of the body) is challenged by a good sneeze or lifting a box, it can leak out a few drops, or up to a tablespoon or more.1 This is SUI, and a decline in estrogen levels plays an important role in its development during menopause, at which time the tissues of the urogenital tract can weaken and become thin.3,4 Additionally, giving birth multiple times, or traumatic vaginal birthing, can contribute to SUI in menopause.4 Gotta go—now!Urge incontinence (UI) is the sudden urge to urinate, often accompanied by urine leakage. In addition to the weakening of pelvic tissues during and after menopause, UI may be caused by a lack of coordination between the brain and bladder, with the signal to urinate being sent by the brain at the wrong time.5Other symptoms of UI include urinating more than eight times per day and more than once at night (nocturia).5 What can be done about urinary incontinence?There are several ways to help make it easier to deal with urinary incontinence. You may start by refraining from alcohol and caffeine; stopping drinking liquids close to bedtime; wearing a disposable pad designed to absorb urine; and maintaining a healthy weight. There are also more comprehensive methods available to address urinary incontinence. Pelvic floor strengthening exercise--The beloved Kegel exercise is a well-known way to help strengthen pelvic floor muscles and possibly eliminate bladder leakage.6 By contracting and relaxing these muscles repeatedly, they can be strengthened and provide better bladder support. Where are your pelvic floor muscles? If you can stop urinating midstream, you’ve found them.6 Ask your healthcare practitioner for information on how to perform the Kegel exercise. Pessary--This small device is inserted into the vagina to help support the pelvic organs and is also used to treat urinary incontinence. Fitted by your healthcare practitioner, a pessary is removable, minimally invasive, and discreet. There are also over-the-counter, disposable bladder supports available that are self-fitting.7,8 Biofeedback--Small sensors are discreetly placed on the body and used to measure what the pelvic floor muscles are doing, as well as provide feedback to help teach you how to control the pelvic floor muscles.9 Medication--Drugs that are designed specifically for urinary incontinence can be used alone or with a method such as biofeedback; they work primarily by relaxing the bladder muscle and increasing the amount of urine the bladder can hold.10 Surgery--While surgery is more invasive than other ways that address urinary incontinence, it can also successfully resolve it. Procedures such as sling surgery and bladder neck suspension can help keep the urethra from moving down and opening accidentally.11 No matter which method you wish to try, always ask your healthcare practitioner about which is right for you. He or she knows your personal health history best and can help you find relief from menopausal urinary incontinence. This information is for educational purposes only. This content is not intended as a substitute for professional medical advice, diagnosis, or treatment. Individuals should always consult with their healthcare professional for advice on medical issues. References:
Fish and shellfish are full of healthy fats, vitamins, and minerals. Great for our physical and cognitive wellbeing, they’re a solid addition to a nutritious diet.1 That said, not all seafood is created equal. This post will outline the differences between farm-raised and wild-caught fish, including their impact on our health and the environment.
What are the differences between farm-raised and wild-caught fish? Fishermen catch wild fish and shellfish in lakes, rivers, oceans, and other bodies of water. These fish eat a natural diet. Farmed fish are bred for human consumption through a process called aquaculture. This means they live outside their natural environment and are generally given processed feed.2 Specifically, farmed fish are placed in pens submerged in ponds, lakes, or even saltwater.1 Some pens are filled with water and kept on land. While this might not sound ideal, fish farming isn’t inherently bad. Sustainable farming practices have become more common than ever, as the World Bank estimates that almost two-thirds of seafood will be farm-raised by 2030. In Norway and Canada, for instance, most farmed salmon are cultivated through an eco-friendly recirculating aquaculture system.3 Here are some other items to consider:
Nutrition: Which fish variety is better for your health? Fish have been shown in clinical studies to display anti-inflammatory properties, not to mention being rich in heart-healthy omega-3 fatty acids.3 The overall quality of seafood, however, depends largely on what fish eat. Wild fish consume a natural diet lower in saturated fats.5 What does this mean? Let’s focus on salmon for a moment. In addition to being higher in saturated fat than wild salmon, farmed salmon contains more omega-3s and 46% more calories. The wild-caught stuff, however, is richer in minerals like potassium, zinc, and iron.4 Consider the following when evaluating both fish varieties for your health:
Most people consume too much omega-6, which may cause inflammation and other symptoms. And farm-raised salmon specifically—despite containing higher quantities of omega-3—has a significantly higher omega-3-to-omega-6 ratio.4 The ratio is still good enough, but it isn’t quite at the level you would find in wild seafood.
Of course, the trace metals found in fish aren’t limited to mercury. Farmed salmon contains higher arsenic levels, while wild salmon contains more cobalt, copper, and cadmium.7 Fortunately, levels of trace metals in both wild and farmed fish are usually so low they’re unlikely to harm the average person.4
Some studies indicate that farm-raised fish have higher levels of contaminants.4 Furthermore, seafood raised via aquaculture may have a higher rate of disease because of some of the farming practices and conditions.5
For example, approximately 530 grams of antibiotics were used per ton of harvested Chilean salmon in 2016. (In contrast, Norway used just 1 gram of antibiotics per ton of harvested salmon in 2008.)4As such, it’s essential that you understand where your fish is from before consumption. Sustainability: Which fish variety is better for the environment? Fish accounts for 17% of our global protein intake.8 For this reason, we can’t rely on wild-caught fish alone. There just isn’t enough wild seafood to keep up with the growing demand. Based on our current trajectory, there’s a global need for another 80 million tons of farmed fish per year by 2050.8 Yet aquaculture may be detrimental to the environment too. Use of antibiotics can cause damage to the environment and adversely affect human health as well.4 Moreover, when lots of fish are crammed together in a small space like a pen, they create a ton of waste that can pollute rivers, lakes, and oceans.8 And the environmental consequences of fish farming doesn’t end there, either. Some fish farms are disease-ridden, which can be toxic to the environment; in Indonesia, shrimp farming specifically has contributed to the decline of the nation’s mangrove forests.8 Since we don’t want to deplete what’s left of our wild fish resources, where does that leave us? Fortunately, some experts say that feeding farmed fish a higher-quality diet free from antibiotics can help address some of the problems described above. Similarly, as fish farmers gain efficiency, governments will be more likely to offer incentives for the adoption of sustainable practices.8 Ideally, the environment will become an even greater focus for everyone in the near future. The verdict on wild-caught vs. farm-raised fish While wild seafood is generally healthier than farmed fish and shellfish, sustainable methods make many farm-raised options completely viable. Both wild-caught and farm-raised fish varieties offer plenty of protein, the omega-3 Docosahexaenoic acid (DHA), and other essential nutrients.4 To make sure you’re eating top-quality seafood, be sure to look into where your seafood is from, and opt to eat local, low-mercury varieties when possible. References:
Consider these general diet descriptions:
So is a vegetarian or vegan ketogenic diet possible? Short answer: yes. The ketogenic diet differs from other diets in that it is not based around food groups you can or cannot eat; rather it is based on the macronutrient ratio your body requires to enter a state of nutritional ketosis (defined by an elevation of blood beta-hydroxybutyrate, the body’s primary ketone body). Thus, any style of eating can potentially be ketogenic, whether that is vegan, paleo, low FODMAP, etc. When you are approaching the ketogenic diet from a plant-based perspective, look at what plant foods comply to the macronutrient ratios you are following and stick to those. General guidelines for following a ketogenic diet:
Vegan ketogenic “food groups”:
Vegan food swaps
Tips & tricks
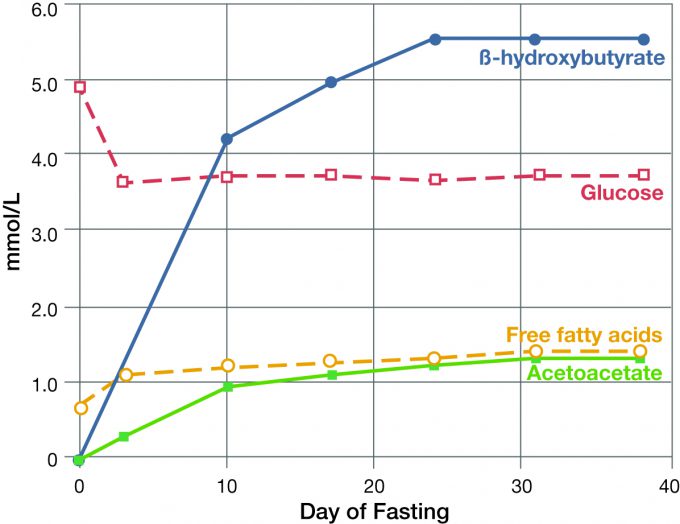
Submitted by the Metagenics Marketing Team Wouldn’t it be nice to live in a world where the answers to all our health questions were black and white, (“Eat this, and you will feel good; don’t eat this, or you will not feel good”)? Unfortunately, health is not black and white, and often we have to navigate through the grey areas to find the truth. MYTH #1: A ketogenic diet increases your risk for cardiovascular diseaseThis myth is centred around the misinformation that saturated fat and cholesterol are the main causes of heart disease. Despite being shown that dietary cholesterol does not raise blood cholesterol1 and saturated fat has little correlation to heart disease,2 there is still a stigma around both. Cardiovascular risk does not boil down to a single biomarker, but rather encompasses a host of factors such as age, sex, total cholesterol, high-density lipoprotein (HDL) cholesterol, triglycerides, smoking, blood pressure, glycemic control, and more. Several of these risk factors may be mitigated by lifestyle changes. Low-density lipoprotein (LDL) cholesterol, as opposed to high-density lipoprotein (HDL) cholesterol, often gets a bad rap because the general understanding about cholesterol is that LDL cholesterol is the “bad” cholesterol, and HDL cholesterol is the “good” cholesterol. While this isn’t entirely misleading, what is misleading is referring to these as absolutes. LDL is usually misrepresented as the single factor that determines one’s risk for cardiovascular disease (CVD), when in fact there is more to the LDL and CVD risk story much of which is still uncovered. The danger lies with the small, dense LDL particles (as opposed to large, buoyant LDL particles),3 which have been shown to be associated with CVD.4 It is not uncommon to see a rise in total LDL levels when following a ketogenic diet. Recently published results of a one-year study of patients on a well-formulated ketogenic diet showed that the ketogenic diet did not change total LDL particle numbers but rather caused a shift toward an increase in large, buoyant LDL particles and decrease in small, dense LDL particles,5 which is a good thing! With all of this said, there is still a lot that is not fully understood about LDL cholesterol in the context of a ketogenic diet. As previously stated, LDL is not the only biomarker to consider when determining risk for CVD. Working with a keto-savvy physician is recommended when considering a ketogenic diet. When part of a weight management program including exercise and lifestyle modifications, the ketogenic diet can actually improve other biomarkers of CVD risk, such as weight,6 HDL cholesterol,6 blood pressure,5 blood levels of saturated fat,7 HbA1c,5 inflammation,8 and more! In fact, research has shown that carbohydrate-rich diets pose more of a health risk than ketogenic diets. High-carbohydrate diets have been associated with increases in small, dense LDL particles and reductions in HDL cholesterol along with raised triacylglycerol levels, all of which contribute to increased CVD risk.9 MYTH #2: The human body requires carbohydrates to survive This one may be hard to wrap your head around considering there are actually some cell types that do have an absolute requirement for glucose and cannot use fats or ketones for fuel, such as red blood cells which lack mitochondria, the organelle required for ketone utilization. Dr. George Cahill, former professor at Harvard Medical School, studied human body fuel metabolism under prolonged starvation, pioneering the understanding of ketones as an alternative fuel source to glucose. His research demonstrated that even after 40 days of fasting, glucose levels in the participants were maintained, despite consuming no food (Figure 1).10 So where does the glucose come from to fuel these cells when carbohydrates are restricted, such as with a ketogenic diet? Once you are keto-adapted (i.e. in a state of sustained nutritional ketosis), there are two primary sources that contribute to glucose maintenance. The first is from amino acids via a process called gluconeogenesis, where certain gluconeogenic amino acids are broken down into glucose. These amino acids can come from the protein consumed or stored in muscles. However, when ketones are circulating in our blood and the brain begins preferentially using ketones for the fuel, glucose requirements are reduced, therefore the need to break down muscle is reduced. This is one way ketones are muscle-sparing. The second source of glucose is from the glycerol backbone of triglycerides. Triglycerides are the storage form of fat and contain one glycerol backbone attached to three fatty acids. When the body breaks down stored fat while in ketosis, the fatty acids are detached from this glycerol molecule to make ketones, and the glycerol molecule can be converted into glucose, accounting for most of the body’s glucose requirements when keto-adapted. Figure 1: Circulating concentrations of βOHB, glucose, free fatty acids, and acetoacetate in obese but otherwise normal man fasting for 40 days. Adapted from Cahill GF et al. Ketoacids? Good medicine? Transactions of the American Clinical and Climatological Association. 2003;114:149-163.
MYTH #3: Nutritional ketosis puts you at risk for ketoacidosis This is one of the most common myths, and despite being proven wrong time and again, people still want to believe that the ketogenic diet causes ketoacidosis. Ketoacidosis is a valid concern given that it can be a life-threatening event where ketone bodies cause a dangerous imbalance in blood pH. However, this condition occurs primarily in those with type-1 diabetes or insulin-dependent type-2 diabetes, and is uncommon in healthy individuals with a fully functioning pancreas. Blood ketone levels are regulated by insulin, just as blood glucose is. When ketones reach their upper limit (~7-8mmol/L), a small amount of insulin is released from the pancreas to help prevent any further elevation in blood ketones, this system is designed to help the body avoid what is considered ketoacidosis (~15-25mmol/L). Nutritional ketosis (i.e. ketosis achieved via a ketogenic diet) is highly unlikely to put a healthy person at risk of reaching dangerous ketone levels. There are rare exceptions to this where ketoacidosis can occur in those adhering to a ketogenic diet in instances such as dehydration, sickness, and possibly pregnancy. However, it is always advised to start a diet and/or weight management program under the supervision of a physician or healthcare provider. MYTH #4: You can’t do keto as a vegan or vegetarian The ketogenic diet is commonly associated with a diet primarily composed of animal fats. However, nowhere is it stated that to follow a ketogenic diet, solely animal fats are required. There are plenty of plant-based fat sources that are highly suitable for a ketogenic diet such as avocados, nuts and seeds, olives, etc., and their oil derivatives. For those people who are vegetarian (but not vegan), the options extend even further to include eggs and dairy, both excellent sources of fats. Incorporating oils will likely be necessary for those following a completely plant-based ketogenic diet, as it would be very difficult to fulfil the macronutrient ratios needed to enter ketosis by utilizing only whole foods. This recent post outlines different types of dietary fats that may be used on ketogenic diet, as many of the sources mentioned in the post are plant-based. There are many low-carbohydrate vegetables that should also be included in a ketogenic diet regardless of whether animal products are part of dietary intake. These primarily include leafy greens, cruciferous vegetables, lettuces, celery, cucumber, and zucchini. There are also many dairy-free alternatives to dairy fats such as nut milks, full-fat coconut milk, nut-based yogurts, and nut-based cheeses, all unsweetened of course! MYTH #5: The ketogenic diet is the same as a low-carb diet Many people begin their ketogenic diet by cutting out carbohydrates and replacing those calories with protein-based foods. Those who are used to restricting dietary fats may approach a ketogenic diet and foods with hesitation. A ketogenic diet is a high-fat, moderate-protein, very low-carbohydrate diet. So, while you may be under the allotted daily grams of carbohydrates, the amount of fats and proteins consumed must be considered as well. Fats contain ~9 calories per gram, while protein and carbohydrates contain ~4 calories per gram. Given this information, portion sizes will likely be reduced when following a ketogenic diet, and this may be more of a psychological barrier than a satiety one. Adding additional fats to meals in the form of oil, butter, ghee, or full-fat dairy can transform a low-carbohydrate meal into a ketogenic meal. Consider adding quality fats to protein sources to slow the digestion of protein and attenuate any glucose/insulin responses that could potentially prevent one from “entering” or “kicking out” out of ketosis. If you are not entering ketosis following what you believe to be a ketogenic diet, void of almost all carbohydrates, you may be over consuming protein. In this case, adjust your macro nutrients to include higher quantities of dietary fats and less low-fat protein sources. Resources:
Disclaimer: This content is not intended as a substitute for professional medical advice, diagnosis, or treatment. Individuals should always consult with their healthcare professional for advice on medical issues. Submitted by the Metagenics Marketing Team Nowadays, thankfully, people are becoming increasingly aware that the low-fat era was one born under a false premise, yet there still seems to be a “fat phobia” lingering among the masses. To clear things up, remembering that “fat ingested does not equal fat stored” may help. This is along the lines of understanding that ingested protein does not automatically equal muscle growth.
In the metabolic state of ketosis, fat is the primary fuel source for the body, and the fat consumed contributes toward fuel for cellular function in much the same way carbohydrates act in glucose burning. Health issues associated with high-fat consumption are, more often than not, due to the combination of both high intakes of fat and carbohydrate, resembling a “Western Diet,” or “Standard American Diet (SAD),” both of which are commonly known to increase risks of obesity and insulin resistance. It is important that these should not be confused with the qualities associated with “good fats.” How did this low-fat idea come to fruition? In the 1950, an American physiologist, Dr. Ancel Keys, hypothesized that consumption of saturated fat raises blood cholesterol levels and results in increased risk of myocardial infarct or heart attack. Over the years, dietary fat was pegged as the main underlying cause for not only heart attacks, but obesity. A new, low-fat food industry was created around the ideology that the “fat you eat is the fat you wear.” Ironically, in the same time that low-fat foods entered the market, the obesity-epidemic was born 1—maybe fat was not the culprit after all? If we only consider the energy-balance equation (i.e. calories in vs. calories out) then it is easy to see how removing dietary fat would be the solution, given that fat contains 9 calories per gram, whereas proteins and carbohydrates contain roughly 4 calories per gram. What is often overlooked, however, are the hormonal responses and satiety factors, among others, associated with consuming fats, carbohydrates, and protein. Of course, calories still matter; you can’t eat more than you burn on the ketogenic diet and continue to lose weight, but it’s time to get over the misconception that consumption of dietary fat leads directly to stored body fat, without considering the other factors at play. How eating fat can lead to burning fat There are many hormones governing our metabolism, but there is one master dietary hormone, and that is insulin. Insulin is released from the beta cells of the pancreas in the presence of glucose (i.e. carbohydrates) to shuttle it away from the blood and into the cells, which lowers blood sugar levels. Insulin is also responsible for telling our cells, “Hey everyone! Glucose is available! There’s no need to breakdown fat for fuel; let’s save that for later!” In the body, carbohydrates are the primary instigator of insulin release, whereas protein only causes a very mild release, and fat causes almost no response. When glucose levels are significantly lowered, such as that achieved with a ketogenic diet, insulin requirements are also reduced. In the absence of insulin, cells can use stored fat for fuel, either directly (e.g. free fatty acids) or indirectly via the generation of ketone bodies (i.e. ketogenesis). Think of insulin as the gatekeeper of fat metabolism: When insulin is present, the gates are closed and fat is trapped inside the cell; when insulin is absent, the gates are open and fat can be broken down for fuel. Keeping your hunger in check on the ketogenic diet Besides suppressing insulin levels, the ketogenic diet is said to be very satiating, suggesting better management and control of the appetite. It can be argued that eating a ketogenic diet allows one to be more in tune with the body’s natural hunger signals. Furthermore, weight loss associated with the ketogenic diet is more often due to the natural calorie deficit that accompanies the diet since the ketogenic diet, by nature, has an appetite-suppressing effect. Leave the roller coasters for the kids! A carbohydrate-based meal often produces a rapid postprandial rise and fall in blood glucose that leaves you searching for more food soon after eating. This happens because of the dependence on glucose for fuel, and when glucose is missing from the bloodstream, it sends the signals to the body that you need food now, sending you to the kitchen. It is almost like being controlled by glucose! Following a ketogenic diet circumvents this glucose/insulin roller coaster in two ways:
The whole “fat makes you fat” myth is just that: a myth. Resources:
There’s been plenty of buzz in recent years around the word “detox,” but your body is not the only thing that can be exposed to toxins. Your whole way of life might be exposing you to emotional toxicity, too.
We take the trash out from our homes on a regular basis. This allows us to discard what’s no longer useful and keep our living spaces clean and pleasant. If we neglect this responsibility, the consequences are hard to ignore: overflowing waste baskets, unpleasant odors, and possibly the invasion of pests! Unfortunately, emotional garbage is not so easy to detect. Bad habits, negative thoughts, toxic people, and unhealthy situations can overwhelm your personal space and accumulate clutter in your mind. Over time, both internal and external stressors cause your mental waste bin to become full. If you aren’t careful to filter out what you don’t need, that waste bin can overflow—and lead to a very unhealthy life! There are plenty of ways to minimize toxicity in your life. Consider these nine steps to start reducing stressors today. 1. Change your self-talk What are you thinking about right now? What did you think about when you first woke up? Believe it or not, your answers say a lot about you and your health.1 Your thought patterns are an integral part of your overall well being. Over time, repeated thought patterns influence behavior and beliefs.1 When your thoughts are mostly negative, it can feel like you’re stuck on a “not-so-merry”-go-round. Remind yourself, too, that you can’t always trust your own thoughts to be impartial. Sometimes you have to hit the pause button, take some deep breaths, and talk yourself off the ledge. And that’s okay. To break free from a negative thought spiral, try a relaxing, rejuvenating activity (e.g., read a book, practice yoga, tend to your garden, or listen to a favorite record) to lift your spirits and get your mind focused on something new. 2. Reevaluate your habits We all have bad habits. Some habits are relatively benign, like biting your nails or smacking your lips when you chew. But others, like hitting the snooze button, comparing yourself to other people, and picking fights with friends or partners, can actually be toxic to your well being. The first step toward improvement is self-awareness. To start, make a list of your habits and mark an X next to the not-so-good ones. As you build your self-discipline, remember to be patient with yourself. Studies say it can take about two months (not 21 days) to make or break a habit!2 3. Walk away from bad relationships Good friendships matter. In fact, research conducted over a ten-year period found that individuals with a stronger network of friends were 22% more likely to outlive their lonelier counterparts.3 But where good friendships can support your health, bad ones can do just the opposite. Pay attention to how you feel after hanging with certain people. If you’re always left feeling distressed in one way or another, it may be best to start distancing yourself from them. Don’t feel obligated to keep up friendships (or romantic partners) that cost you your mental and emotional sense of peace. 4. Disconnect from social media Social media is a double-edged sword. On one hand, it helps us stay connected with friends and family. On the other hand, it’s a hotbed of competition, comparison, and drama. Taking a break from social media can clear mental clutter and help you focus on the here and now. Evaluate your feelings after using Facebook, Instagram, or any other social network, then ask yourself why you feel this way. It’s a good idea to delete or un-follow highly negative people or those who stir up bad feelings whenever you visit their pages or see their posts. Doing this can spare you those negative emotions and allow you to focus your energy on more positive things. If nothing else, social media can be a real time killer. The time you save on scrolling could mean more time spent on hobbies or with loves ones. 5. Downsize your wardrobe Clothes are a necessity and a fun way to express personal style. Unfortunately, they are also an easy thing to hoard. Physical clutter can lead to mental clutter. If sartorial clutter has taken over your bedroom, you may be in need of a closet purge. The clothes you wear can affect your mood and your confidence, so it’s important that you feel good in them. Are any of your duds, well…a dud? Find out by doing a quick survey of every item in your wardrobe. Ask yourself: Would I feel good wearing this tomorrow or to an upcoming event? If the answer is no, it may be time to let it go. If you choose to donate, you can feel good knowing that your preloved apparel might work equally well for someone new. 6. Reorganize your work space While the importance of keeping a clean home seems like a no-brainer, your work area can be an easy thing to neglect—until you find it’s covered in “organized” piles of paper and old business cards. According to science, a clean, organized work space can boost productivity. In fact, a Harvard study found that students who worked in a tidier environment remained focused for 7 ½ minutes longer than messier students, who were more likely to experience frustration and weariness.4 Giving your desk or work space a weekly once-over means you are less likely to be invaded by dust bunnies and more likely to check items off your to-do list. 7. Turn off the TV It’s easier than ever to get hooked on television. The average American adult watches five hours of TV per day (wow!), and about 50 percent of Americans use some kind of streaming service—a number that’s been steadily rising.5 As statistics show, what we spend much of our free time doing is more passive than active, and that mindset may spill over into other areas of life. Although entertainment is not all bad, moderation may be the best approach to screen time. Increased television watching is associated with lower physical and mental vitality and may be linked to chronic health conditions.6,7 If this feels relevant for you, consider cutting your quality time with the tube by a small amount each day. Replace that time with a physical activity or creative hobby, which—according to research—can promote overall well being 8. 8. Reassess your diet The benefits of a balanced diet go beyond your physical body. It can also make you feel good mentally. Eating foods rich in vitamins, minerals, and antioxidants can protect your brain from oxidative stress, support brain function, and help stabilize your mood.9 There’s also plenty of evidence showing that when your body is low in certain essential nutrients, such as vitamin D and omega-3's, it can negatively impact mental health.10,11 If you’re stuck in a funk, your diet may be playing a role. To help combat those blues and support your health, start by incorporating wholesome snacks into your day, like nuts, fruit, or string cheese, and eat plenty of nutrient-dense greens whenever possible. Stock your fridge or pantry with things you enjoy that won’t make you feel guilty. And to set yourself up for success, rid your kitchen of sugary, greasy snack foods so you won’t be tempted to indulge. 9. Keep a journal Had a bad day? Feeling low but you don’t know why? Write about it! Reading what you wrote a few days later may give insights on things that can be reduced or eliminated to avoid future bad or unhappy days. Writing is one of the best ways to release bad feelings. Writing down your thoughts can feel just as good as venting to a friend. And because your thoughts are recorded in one place, it’s much easier to pick up on patterns in your thoughts and behavior—helping you prioritize problems, identify triggers, and work through anxious feelings.12 Anyone can do it! When life gets too complicated, well being silently suffers. And though we all have different thresholds for toxic overload, most of us could benefit from taking some steps to detox our lives as well. References:
Add These Detoxifying Foods to Your Shopping List
Detox is a hot topic nowadays. Many detox programs promise to cleanse your body harmful compounds, and others tout weight loss and additional health benefits. Unfortunately, many of these detox methods involve a major dietary overhaul or giving up solid foods altogether, which may actually be harmful to your body.1 Because your body is in constant detox mode, you can encourage this process, correctly and effectively, by simply eating the right foods. Scientific research has found that the nutrients, enzymes, and antioxidants found in certain whole foods can help support the liver’s detoxification pathways, prevent the buildup of toxins, and support overall health.2-4 Chemicals and toxins are everywhere, but your body is built to fight back. Here are six of your top nutritional allies: 1. Cruciferous vegetables & leafy greens Spinach, broccoli, and Brussels sprouts are among the folate- and chlorophyll-richgreens that support the body’s detoxification process by helping to detoxifythe blood and cleanse the intestines.2,4-7 All the more reason to go green! Broccoli deserves some special attention for its high concentrations of glucoraphanin, which is converted in the body to sulforaphane—an active compound associated with many positive health benefits, including its role in inducing phase II detoxification enzymes and support for overall liver health.8-10 2. Turmeric Used in many anti-inflammatory and detoxifying recipes, turmeric contains a powerful substance called curcumin, a polyphenol with anti-inflammatory and antibacterial properties. Science has found curcumin to play a role in modulating cellular response to oxidative stress—demonstrating hepaprotective and therapeutic effects on liver health.11,12 3. Sesame Commonly used in bread products, oils, and dressings, sesame is flowering plant that maybe beneficial for detox. Sulfur-containing amino acids methionine and cysteine—both of which are found at high levels in sesame—are precursors to the production ofglutathione, a key antioxidant in the detoxification process.4 4. Beets These pretty-colored veggies contain betanin, which can help repair liver cells and help support detoxification processes in the liver.13,14 It’s also great for digestion. Tell toxic chemicals to “beet” it! 5. Guacamole No party spread is complete without it! Avocado has high concentrations of the antioxidant glutathione, which has been found to neutralize free radicals to support and protect the liver—i.e., your detoxification powerhouse.4,15,16 Why guacamole? Avocado in this form often uses other healthful ingredients, like cilantro. Also known as coriander, cilantro contains oils with antibacterial, antifungal, and antioxidative properties.17 Pass the guac, please. 6. Garlic Alongside its knack for warding off vampires, garlic may be beneficial for clearing out toxins. The sulfur-containing compound allicin, which gives garlic its unique and strong-smelling aroma, may enhance antioxidation and detoxification capabilities18,19 and has also demonstrated hepatoprotective effects against heavy metals in the liver.20 Incorporating more of these foods into your diet can help support detox processes. Add them to your shopping list today! References:
|
Categories
All
Archives
April 2024
|
|
Join Our Community
|
|
Amipro Disclaimer:
Certain persons, considered experts, may disagree with one or more of the foregoing statements, but the same are deemed, nevertheless, to be based on sound and reliable authority. No such statements shall be construed as a claim or representation as to Metagenics products, that they are offered for the diagnosis, cure, mitigation, treatment or prevention of any disease. |













 RSS Feed
RSS Feed