|
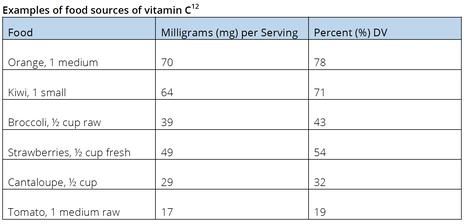
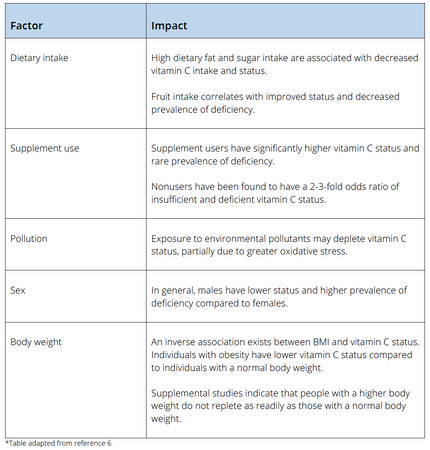
by Cassie Story, RDN Abstract: Although it was not identified and isolated until the 1930s, vitamin C has been known to protect against and treat certain disease states since the 18th century. Ask any health care practitioner to recall the first nutrient deficiency they learned about, and vitamin C will likely top the list. Images of sailors in the 1700s returning to shore with bleeding gums, fatigue, and even death due to a deficiency in this potent, water-soluble, antioxidant micronutrient likely come to mind. Ask any consumers what nutrient they should take during cold and flu season to help minimize their risk of infection, and once again, vitamin C will typically be their reply. For these reasons, vitamin C is arguably one of the most famous micronutrients. This post will dive into the role of vitamin C within the body and the potential health benefits of optimal intake and review considerations for its impact on the immune and respiratory systems. Function of vitamin C in the body Unlike most animals, due to the result of random genetic mutations, humans have lost the ability to synthesize ascorbate in our livers, making vitamin C an essential micronutrient.1 This important antioxidant serves many functions in disease prevention and optimal health status. Vitamin C is involved in protein metabolism and is required for the biosynthesis of certain neurotransmitters, as well as L-carnitine and collagen. It also serves as a cofactor for several enzyme reactions.2 Mild insufficiency, or hypovitaminosis C, has been associated with low mood, and more severe deficiency can lead to the clinical syndrome of scurvy, a condition that remains diagnosed in individuals today—and has played a role in global public health outbreaks.3,4 As vitamin C is a regenerative antioxidant, research continues to evaluate the impact of vitamin C and its role in reducing the destructive effect of free radicals. This may assist in the prevention of or delay in certain cancers, cardiovascular disease, and other conditions where oxidative stress affects human health.5 Not only does vitamin C have biosynthetic and antioxidant functions, it plays an important role in immune function and assists in the absorption of nonheme iron. Vitamin C absorption and status Vitamin C concentrations are tightly controlled within the body. Despite this, studies indicate that hypovitaminosis C and deficiency exist worldwide. Hypovitaminosis C is prevalent within certain populations in developed countries, including individuals with obesity, those who smoke, and people with low fruit and vegetable intake—and is the fourth leading micronutrient deficiency in the United States.6 Dietary intake is a primary factor in an individual’s vitamin C status. The amount consumed and frequency of consumption correlate well with plasma status and deficiency risk.6 Well absorbed in small quantities (i.e.: 200-400 mg at a time), through sodium-dependent vitamin C transporter-1 (SVCT-1), the enterocyte is rapidly saturated, and vitamin C is then transported, at varying concentrations, to several body tissues.7 Many organs have concentration-dependent mechanisms to retain vitamin C during situations where supply is low, namely brain tissue and adrenal glands.8 Plasma saturation occurs at a concentration between 70-80 µmol/L, although typical laboratory assessment methods prove highly susceptible to inaccuracies—leaving it challenging for many clinicians to assess accurate vitamin C status in their patients.8 Factors that impact vitamin C status6 Recommended intake and sources Population-based studies indicate that a majority of Americans meet the recommended dietary allowance (RDA), which is 90 milligrams (mg) per day for males and 75 mg per day for females, although ideal intake and serum concentrations have been a topic of debate for health experts around the world, and recommended values are not universal.9 A range of identified health benefits have been observed at higher intake levels. This has led a number of international agencies to increase their dietary recommendations, as the previous recommendations were based on the low level needed to prevent scurvy, which is estimated to be 10 mg per day.9 Despite its popularity among health care professionals and consumers, average US adult intakes are estimated to be 105 mg for males and 84 mg for females.10 While it is apparent that most individuals meet the RDA, many do not achieve the estimated optimal intake needed for its positive biological impact—which is speculated to be much higher, with many experts suggesting a daily intake of 200 mg for optimal health.11 Food sources Fresh fruit and vegetables are the main contributors of dietary vitamin C, with fruit intake correlating strongly with plasma vitamin C levels.6 Major contributors of vitamin C in the typical American diet are potatoes, citrus fruit, and tomatoes. Foods rich in vitamin C include oranges, kiwi, berries, papayas, mangos, melons, spinach, asparagus, and Brussels sprouts.12 Impact of vitamin C supplementation Supplemental use Five or more servings of fruits and vegetables per day can often lead to an optimal daily vitamin C intake of 200 mg, with special attention to one or two servings coming from a high-vitamin C source. This is not always possible, and taking supplements—in addition to dietary intake, can help to achieve and maintain optimal status.
Dietary supplement sources The majority of dietary supplements provide vitamin C in the form of ascorbic acid, which has an equivalent bioavailability to the naturally occurring ascorbic acid found in food sources.16 Other forms of supplemental vitamin C include mineral ascorbates, liposomal-encapsulated, or combination products. The upper limit has been set at 2,000 mg per day, due to the potential of diarrhea or other gastrointestinal (GI) effects, not due to a potential toxic impact. Buffered forms have been shown to help prevent GI distress and offer higher absorption than traditional ascorbic acid, possibly related to the presence of other minerals and amino acids. One study on 22 healthy subjects found that a buffered form of vitamin C improved absorption in healthy individuals by 18-25% when compared to ascorbic acid.17 Immune, inflammation, and respiratory impact Vitamin C appears to play a role in both prevention and treatment of respiratory and systemic infections by boosting several immune cell functions.18 Vitamin C status may be depleted by various disease states due to inflammatory processes and greater oxidative stress. During times of active infection, requirements for vitamin C increase with the severity of the infection—which requires significantly higher intakes to reach normal plasma status to make up for the added metabolic demands.6 Prophylactic prevention, on the other hand, advises that dietary intake is, at minimum, adequate. However, in order to achieve plasma saturation and optimize cell and tissue levels, doses of 100-200 mg per day are suggested.18 The role of vitamin C in immune defense and inflammation is multifactorial. It plays a role in inflammatory mediators by modulating cytokine production, decreasing histamine levels, and offering protection of key immune enzymes. Apoptosis, the necessary programmed cellular death of neutrophils, supports the resolution of inflammation and helps to prevent extreme tissue damage. Caspases are oxidant-sensitive, thiol-dependent, key enzymes in the apoptotic process. Vitamin C is thought to protect the caspase-dependent apoptotic process following the activation of neutrophils. Numerous studies have found weakened neutrophil apoptosis in patients with severe infection when compared to control groups. Animal studies have shown that administration of vitamin C greatly reduced the numbers of neutrophils in the lungs of septic animals.18 Cytokines, cell-signaling molecules secreted by certain immune cells, respond to infection and inflammation and can elicit a pro- or anti-inflammatory response. Vitamin C has been found to regulate systemic and leukocyte-derived cytokines in a multifaceted way. Preclinical, in vitro and animal studies have shown both positive and unfavorable effects of incubation with vitamin C. The effect of vitamin C seems to depend on the cell type and/or the inflammatory stimulant but overall appears to assist in normalizing cytokine generation.18 Following chemical exposure, natural killer (NK) cell function, as well as T and B cell function, decreases and can remain low for several weeks to months.17 Studies have shown enhanced immune function and improvement in NK cell function after oral doses of buffered vitamin C, as well as T and B cell function improvement following toxic chemical exposure. One study, of 55 subjects, used individualized dosing (60 mg/kg of body weight) of buffered vitamin C to evaluate the impact of high-dose vitamin C following a toxic chemical exposure and found that functional immune abnormalities can be restored following such an event.19 Allergies and the common cold Histamine, an immune mediator, is produced in response to pathogens and stress. Vitamin C depletion is associated with higher circulating levels of histamine. Intervention studies with supplemental oral vitamin C (range 125 mg–2 g/day) have found a decrease in histamine levels; however, they have been more impactful in patients with allergic symptoms compared to infectious diseases.18 The impact of vitamin C intake on common cold incidence has been an area of interest for the last 50 years.20 Meta-analyses have indicated that supplementation with 200 mg or more per day is effective in reducing the severity and duration of the common cold, and in individuals who have inadequate vitamin C status, vitamin C supplementation may decrease the incidence of the common cold. Thus, it appears that taking high-dose supplemental vitamin C daily during cold and flu season may reduce the risk of cold duration and severity.21 Respiratory impact Exposure to air pollution oxidants and tobacco smoke can alter the oxidant-antioxidant balance in the body and lead to oxidative stress.22 When vitamin C levels are insufficient, antioxidant defenses are impaired and can further compound the impact of oxidative stress within the body. Environmental oxidants can damage the respiratory tract lining fluid and increase the risk of respiratory disease. Vitamin C acts as a free-radical scavenger that can scavenge superoxide radicals and oxidant air pollutants—and its antioxidant properties offer protection to lung cells exposed to oxidants caused by various pollutants, heavy metals, pesticides, and xenobiotics.23 Vitamin C also plays a role in proper endothelial function, and deficiency has been associated in pulmonary arterial hypertension.24 Patients with acute respiratory infections have been found to have low plasma levels of vitamin C, and supplementation has been found to return plasma levels to normal and decrease the severity of respiratory symptoms. Beneficial effects of vitamin C supplementation on recovery of respiratory infections, including pneumonia, have been identified. Studies on hospitalized patients with pneumonia have found that supplemental vitamin C at a low dose (250-800 mg/day) reduced length of stay by 19% compared to those without vitamin C supplementation. Those that were given higher doses (500 mg–1.6 g per day) had an even greater reduction at 36%.18 It appears that low vitamin C levels seen during respiratory infections are both a source and a result of the disease. Respiratory health case study10 In a recent case study, a man in his 60s experienced shortness of breath and swelling of the legs associated with a frank vitamin C deficiency, which was attributed to a diet low in vitamin C and no supplemental intake. He was treated with supplemental vitamin C at 1,000 mg twice daily; his symptoms resolved after five months on this treatment plan.
Genetic variants Recent discoveries in genetic variants’ influence on vitamin C status have been found. Several single-nucleotide variants have been identified in the SLC23A1 gene, which encodes SVCT-1 and is responsible for the active uptake of dietary vitamin C and the reuptake of filtered vitamin C in the kidneys. In vitro data for this variant indicates a 40-75% decrease in vitamin C absorption from the gut and has been shown to present in 6-16% in those of African descent.25 A common variant of the hemoglobin-binding protein haptoglobin (Hp2-2) influences the metabolism of vitamin C. In vitro studies have found that this alters the ability to bind to hemoglobin and leads to an increase in oxidation of vitamin C.26 The Hp2-2 variant seems to have a greater impact on individuals with dietary intakes of less than 90 mg of vitamin C per day.27 Individuals with genetic variants that influence vitamin C status may require even higher dietary intakes. Luckily, high-dose vitamin supplementation has been found to amend certain gene-variant defects.28 Conclusion A majority of individuals would benefit from increasing fruit and vegetable intake to improve overall nutrition status, including vitamin C. Ensuring adequate intake of vitamin C through diet and with the use of supplementation is important for proper immune function and resistance to infections. This is especially critical for individuals with certain genetic SNPs or other lifestyle factors that may lead to a decline in vitamin C status. Citations
Cassie I. Story is a Registered Dietitian Nutritionist with 17 years of experience in treating metabolic and bariatric surgery and medical weight loss patients. She spent the first decade of her career as the lead dietitian for a large volume clinic in Scottsdale, Arizona. For the past seven years, she has been working with industry partners in order to improve nutrition education within the field. She is a national speaker, published author, and enjoys spending time with her two daughters hiking and creating new recipes in the kitchen!
0 Comments
Leave a Reply. |
Categories
All
Archives
April 2024
|
|
Join Our Community
|
|
Amipro Disclaimer:
Certain persons, considered experts, may disagree with one or more of the foregoing statements, but the same are deemed, nevertheless, to be based on sound and reliable authority. No such statements shall be construed as a claim or representation as to Metagenics products, that they are offered for the diagnosis, cure, mitigation, treatment or prevention of any disease. |


 RSS Feed
RSS Feed